Facts About Donation
Prior to the S. C. Organ and Tissue Donor Registry launch on December 23, 2008, approximately 1.2 million South Carolinians had the red heart symbol on their driver’s licenses/IDs. This represented 34% of residents with driver’s licenses/IDs. The original heart with a “Y” was only a symbol of an individual’s desire to become a donor, but was not a registry. No one could be transferred into the newly created registry. The challenge is to reach the people who already believe they are in a registry in addition to those who have never considered donation in the past.
Registering is easy, quick, and heroic. Individuals can register now on this web site or by obtaining, renewing, or changing their S.C. driver’s license/ID at any SCDMV office. When registering through the SCDMV, a new logo representing legal consent will be placed on an individual’s license/ID. It is a heart and “Y” surrounded by a circle with 11 “ticks” in it. This represents the fact that nationally every 11 minutes another person is added to the transplant waiting list.

Donate Life South Carolina is the nonprofit organization mandated by South Carolina Legislation to maintain the South Carolina Donor Registry. This registry is dedicated to saving the lives of the many South Carolinians awaiting life-saving transplants.
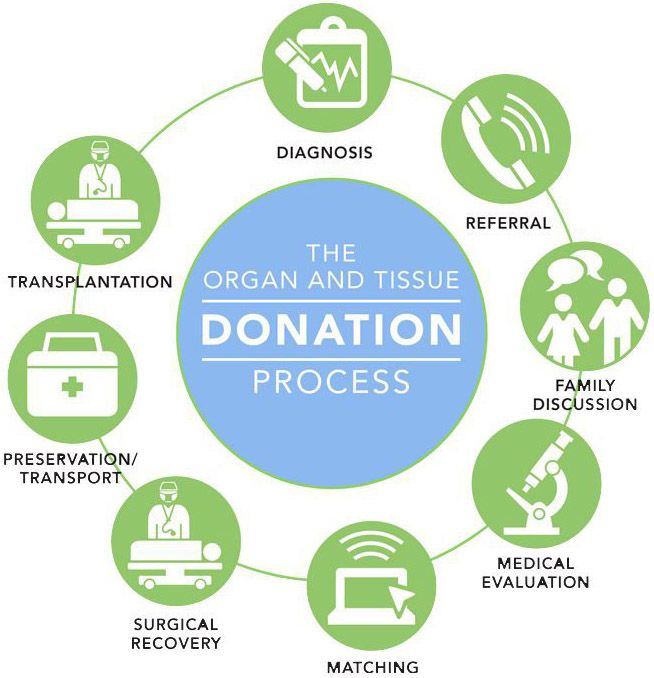
The Donation Process
Organ, eye, and tissue donation involves a complex series of events requiring teamwork among physicians, nurses, hospital staff and procurement and transplant teams. The four major steps that generally define the donation process are outlined below. The significant activities (in bold) will always occur, but the sequence and time frame may vary depending on individual circumstances. The process can vary from a few hours up to more than 20 hours.
8
The number of lives your organ donation could potentially save
2
The number of people you could restore vision for with your cornea
75
The number of people you could heal with your tissue
STEP 1
Identification & Referral
-
Pronouncement of death after evaluation, testing and documentation by the appropriate physician
-
Referral to procurement organization for initial evaluation
-
Death explained to the family
-
Evaluation of patient’s chart and key information by Organ Procurement Organizations (OPO)
STEP 2
Consent
-
Individuals over 18 who are listed on the Donor Registry are considered first person consent – go to 3 below
-
Individuals under 18 require family/guardian consent
-
1. Donation options discussed with family
-
2. Consent forms signed and witnessed
-
3. Medical/Social History obtained from family
-
4. Medical Examiner/Coroner’s release obtained for donation
STEP 3
Evaluation & Maintenance
-
Test for contagious diseases
-
Evaluate organ and tissue stability and suitability
-
Stabilize hemodynamic functions
-
Identify recipients for organs
STEP 4
Recovery
-
Mobilize transplant teams
-
Operating Room organ recovery procedures begin
-
Preservation and procurement of organs
-
Eye and tissue recovery follow organ recovery
-
Autopsy and/or release of body
-
For further information about the donation process go to South Carolina’s Organ Procurement Organization’s website
Myths and Misconceptions
Some people do not wish to be donors because of incorrect or misleading information they have seen, heard or read. We want to be sure your decision about organ donation is based on the facts. Get the facts behind some of the more common misconceptions about donation.
Myth: Wealthy people and celebrities are moved to the top of the list ahead of “regular” patients.
Fact: The organ allocation and distribution system is blind to wealth or social status. The length of time it takes to receive a transplant is governed by many factors: blood type, patient size, time on the waiting list, severity of illness and other medical criteria. Factors such as ethnicity, gender, age, income or celebrity status are not considered when determining who receives an organ.
Myth: My religion does not support organ donation.
Fact: No major organized religion in the world objects to organ donation for specific views, click here. In fact, donation is often encouraged as an act that exemplifies a basic religious principle – that the giving of life and alleviation of pain and suffering is the highest level of spiritual generosity and love one can offer.
Myth: The donor family incurs cost for organ donation.
Fact: Families of donors are in no way responsible for costs relating to organ and tissue donation. Those costs are paid by the organ donor recovery program and later billed to the transplant center, which in turn bills the transplant recipient’s insurance company. Donor families pay only for medical costs up to the time of their loved one’s death.
Myth: Regular funeral services are not possible following organ donation because donation will mutilate the body.
Fact: While donation may delay funeral arrangements for up to 36 hours, regular funeral and memorial services can be planned. In most cases, organ, tissue, and eye donation does not interfere with an open casket viewing. Before moving forward with a procedure we provide information to families and answer their questions to ensure we fully understand their wishes. The recovery of organs, tissues, and eyes is performed by qualified surgeons and recovery staff in a sterile environment. As in any other surgical procedure, the body is treated with the utmost respect and care
Myth: I am too old to be a donor.
Fact: There is no age limit for donation. At the time of death, appropriate medical professionals will determine whether organs and tissues are useable for transplantation. Recovery for research, therapy, and whole body donation are possible options.
Myth: I have a history of medical illness, so you would not want my organs or tissues.
Fact: At the time of death, appropriate medical professionals will review your medical and social history to determine whether or not you can be a donor. With recent advances in transplantation, more people than ever before can be donors.
Myth: I don’t need to register to be a donor or tell my family that I want to be a donor, because I have it written in my will.
Fact: By the time your will is read, it will be too late to recover your organs. Registering to be a donor and telling your family about your decision is the best way to ensure your wishes are carried out. You may also designate donation in an advanced directive or in a health care power of attorney where you designate someone to make decisions if you are not able.
Myth: Organs for transplant can be bought and sold on the black market.
Fact: Unlike some third world countries where an individual can sell one of his/her kidneys for transplant, the selling or buying of organs for transplant is illegal in the United States. There is no transplant physician or center in this country that will transplant an organ that was not recovered through the national waiting list system.
Myth: A physician or EMT may not do everything possible to care for me in an emergency situation in order to take my organs for transplant.
Fact: Upon arrival at an accident scene or upon receiving you in the emergency room, all medical personnel immediately spring into action to try and save your life. Physicians involved in a patient’s care by law have nothing to do with transplant programs. Death can be declared only by following strict medical and legal guidelines and usually with the input of more than one physician. The local organ procurement organization does not become involved until all lifesaving efforts have failed and death has occurred.
Myth: It doesn’t matter what I decide about donation, because my family will make the final decision.
Fact: The S. C. Code states that family permission is not required for donation, and your decision to donate will be honored. It is helpful to talk to your family about your donation decision so that they may assist in carrying out your wishes.
Myth: I am donating my entire body to science so I will also be an organ and tissue donor.
Fact: A body that is donated for scientific research cannot be used for organ and tissue donation, except in the case of corneas.
Myth: Someone might take my organs before I am really dead.
Fact: Donation can only occur after there is an official declaration of death based on the laws in that jurisdiction.
